Disc Injuries and Laser
- May, 01, 2017
- Trenton Talbitzer
- Back Pain, MLS Laser
- No Comments.
Disc Injuries and Laser Treatment
Low back pain has obvious lifestyle and financial burdens; when it is accompanied by radiation of pain and numbness in the lower extremities, it can be truly debilitating. Lumbar disc herniations account for only 4 percent of low back pain patients but account for a high percentage of low back pain costs.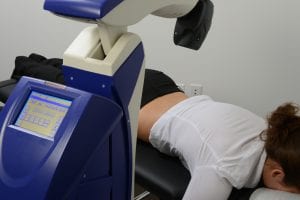
A painful disc herniation results when a tear of the annulus fibrosus allows migration of the nucleus pulposus (protrusion), resulting in nerve root irritation. Lumbar disc herniations typically occur in individuals between the ages of 30-40 years, 1-2 when the nucleus pulposus is still fluid and the annulus is weakened by strenuous activity and age. Due to this relatively young demographic, poor treatment outcomes can result in decades of suffering for these patients.
Prior to the existence of imaging studies, little was known about the healing mechanism of disc herniations. Imaging studies have confirmed what has been long suspected: Disc herniations can decrease in size and even disappear spontaneously, leading to the absence of pressure on the nerve root.
In adult discs, blood vessels are normally restricted to supplying only the outer layers of the annulus. Low oxygen tension at the center of the disc leads to an anaerobic metabolism, resulting in high concentrations of lactic acid and low pH. These deficiencies in metabolite transport limit both the density and metabolic activity of disc cells. Collagen turnover time in articular cartilage is approximately 100 years and is theorized to be even longer in the disc. The result is that intervertebral discs have a limited ability to recover from metabolic or mechanical injuries such as herniations.
There have been a number of mechanisms investigated in attempts to determine how disc herniations heal. It is generally accepted that the herniated disc fragments are reabsorbed. Histological investigations have shown the presence of granulation tissue with abundant vascularization surrounding the fibrocartilaginous fragments. Within the granulation tissue, the prevailing cell types are macrophages with fibroblasts and endothelial cells. These cell types have been demonstrated to be positively affected by laser therapy. The stimulation of macrophages and fibroblasts could be the primary mechanism by which laser therapy heals disc herniations.
Inflammatory markers such as IL-1, IL-6 and TNF-a are also present at the site of disc herniations, leading to higher prostaglandin E2 concentrations. Two studies have demonstrated that laser therapy is effective in reducing prostaglandin E2 concentrations. Bjordal has demonstrated that inflammation is greatly reduced 75, 90, and 105 minutes after active laser therapy compared to levels prior to treatment. The reduction in inflammation appears to be another method by which laser therapy promotes healing in disc herniations.
There is substantial published research on the effectiveness of laser therapy in treating LBP and lumbar disc herniations. The majority of these research articles discuss chronic (nonspecific) low back pain either alone or with exercise. These positively inclined studies seem to be absent in reviews from either the American Pain Society / American College of Physicians or the Cochrane Collaboration indicating that all publications are suspect in varying degrees.
In the review of laser therapy for low back pain performed by the American Pain Society / American College of Physicians, four trials (566 patients) demonstrated that laser therapy was effective and one trial (140 patients) found laser therapy to be no more beneficial than a sham laser device. The conclusion from this review was: “Non-invasive therapies (low-level laser therapy) have not been shown to be effective for chronic, sub-acute or acute low back pain.” A letter to the authors regarding their bias against laser therapy and in support of pharmaceuticals only prompted the authors to downgrade the evidence supporting acetaminophen and cite the Cochrane study to support their stance on laser therapy.
The Cochrane study they refer to found that “three high quality studies (168 people) separately showed statistically significant pain relief with laser therapy in the short-term (less than three months) and intermediate term (less than 6 months) when compared with sham laser therapy.” Two small trials (151 people), also included in the Cochrane review, independently found that the relapse rate in the laser therapy group was significantly lower than in the control group at six-month follow-up. The conclusion was that “based on these trials, with a varying population base, laser therapy dosages and comparison groups, there is insufficient data to either support or refute the effectiveness of laser therapy for low back pain.”
The resounding statements from both of these meta-analyses were that “more studies are required” and “larger trials on specific indications are warranted.” Lacking in the conclusions were any suggestion of “how many patients and studies” are required to provide sufficient evidence. A recent study examining the effectiveness of laser therapy in treating lumbar disc herniations measured by clinical evaluation and magnetic resonance imaging (MRI) found that “low power laser therapy is effective in the treatment of patients with acute lumbar disc herniations.”
Invariably, studies provoke questions. Some of the more common parameters for consideration are the duration and extent of laser therapy, joules per centimeter square of irradiation, power settings, etc. One must conclude these studies and meta-analyses, although well-intentioned, may in many instances be misguided. In our experience, almost 40 percent of all patients presenting for treatment at our clinic suffer from back problems characterized by severe pain, and over 85 percent can be treated successfully with laser therapy.
The financial justification for the use of laser therapy as the first line of defence in disc herniations is overwhelming. Data collected from the SPORT trial found that the average surgical procedure cost $15,139, which rises to $27,341 when other costs such as diagnostic tests and missed work are factored in.21 The cost of conservative treatment in that same study averaged $13,108. In our experience, even the most extreme example of a herniated disc patient (receiving 40 treatments), resulted in a total treatment cost of just $3,200. When diagnostic tests and health care visits are factored into this equation, the total cost of laser therapy is closer to $5,700. This is a savings of more than $20,000 versus surgery and $7,500 over standard conservative treatment. Moreover, laser therapy is noninvasive and no adverse events have been reported in more than 3,000 publications.
In summary, this review of the current literature clearly reveals some of the shortcomings of meta-analyses and the performance of studies without standardized methodologies. We conclude that medical convention has demonstrated that the relief of symptomatic disc herniations continues to be problematic and that both conservative and surgical solutions in the majority of cases appear to be equally ineffective. While the application of appropriate therapy requires a comprehensive understanding of the anatomy, pathology and biomechanics of the spinal column, we feel that laser therapy presents the most logical and effective therapeutic approach in managing these pervasive medical conditions.
- Allergy Relief (5)
- Autoimmune (3)
- Back Pain (7)
- Chiropractic (9)
- Food Info (3)
- Health Tips (9)
- Internal Medicine (13)
- MLS Laser (5)
- Nutrition (3)
- Office Information (2)
- Recipes (4)
- Testimonials (6)

Leave a Comment